Understanding the Role of a Corneal Transplant
A corneal transplant is a surgical procedure that replaces a damaged or diseased cornea with a healthy donor cornea. The cornea, the transparent front layer of the eye, is essential for focusing light and enabling clear vision. When the cornea becomes scarred, thin, or irregular, vision can be severely impaired. Conditions like keratoconus, corneal dystrophies, infections, and injuries often make a transplant necessary. Corneal transplantation is considered when other treatments, including medications or specialized lenses, are insufficient. Modern techniques have significantly improved the safety and success of these procedures. Patients can often experience remarkable improvements in vision, quality of life, and daily functioning. Understanding what a corneal transplant involves is crucial for anyone considering this procedure.
Common Eye Conditions That Require Corneal Transplant
Several conditions can lead to the need for a corneal transplant. These include:
- Keratoconus, which causes the cornea to thin and bulge into a cone shape
- Scarring caused by infections, injuries, or previous surgeries
- Corneal dystrophies, which are inherited disorders affecting the cornea’s clarity
- Corneal swelling due to endothelial dysfunction
- Severe thinning or perforation of the cornea
- Chemical or thermal injuries that damage the corneal tissue
Early diagnosis and treatment of these conditions can improve the chances of a successful transplant. Ophthalmologists assess each case individually, considering age, general health, and lifestyle factors. Patients are also evaluated for any other eye conditions that may impact the procedure’s success. Thorough assessment ensures the best possible outcomes and minimizes potential complications. Awareness of these conditions allows patients to take timely action to protect their vision.
Preparing for Corneal Transplant Surgery
Preparation is a critical step for a successful corneal transplant. Patients typically undergo detailed eye examinations, including corneal mapping, thickness measurements, and visual acuity tests. Any active infections or inflammation must be treated before surgery. Doctors may advise adjusting certain medications that could affect healing. Maintaining a healthy lifestyle, including proper nutrition and avoiding smoking, supports recovery. Patients are encouraged to understand the procedure and ask questions to reduce anxiety. Emotional preparation is also important, as knowing what to expect improves compliance with postoperative instructions. Proper preparation contributes to a smoother surgical experience and faster recovery.
What to Expect During the Surgery
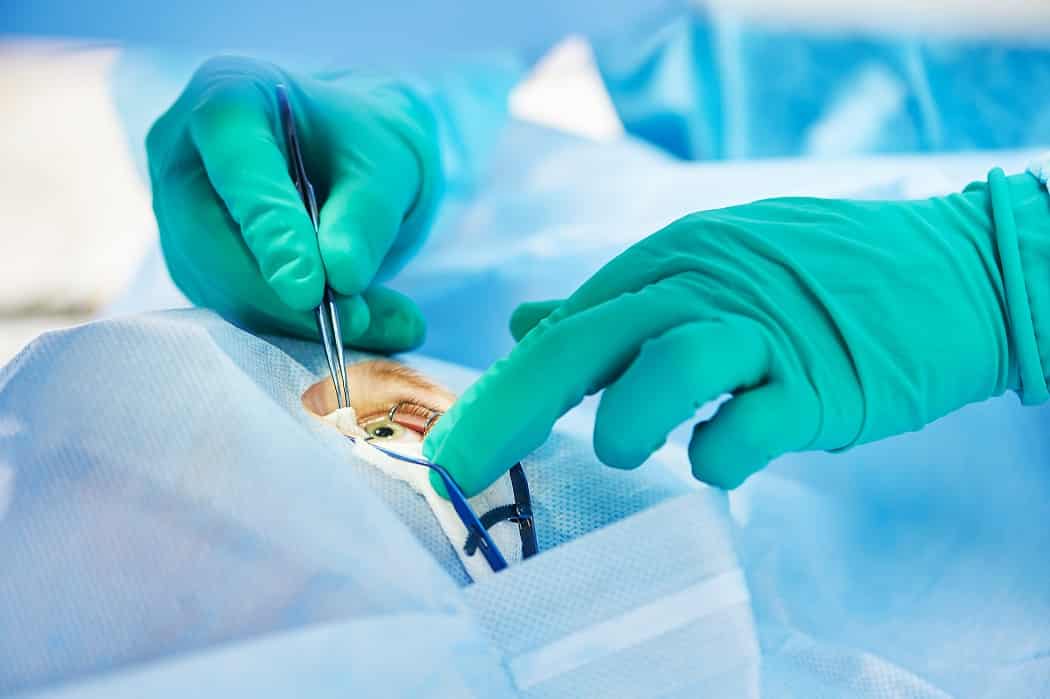
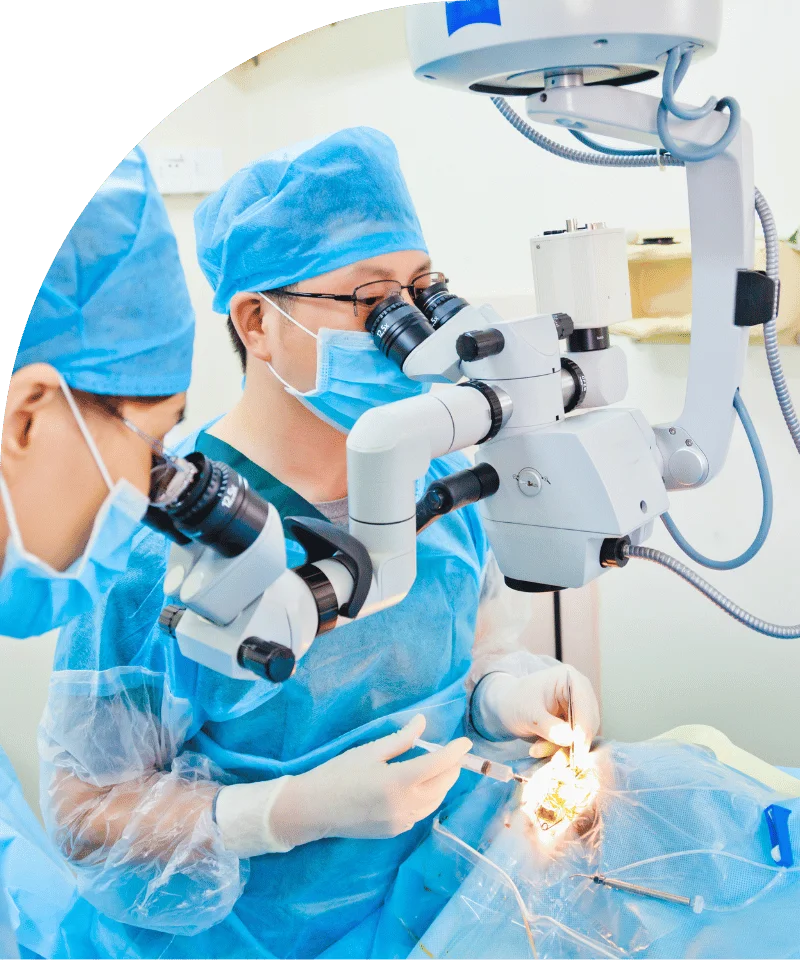
During corneal transplant surgery, the damaged cornea is carefully removed and replaced with healthy donor tissue. The procedure can be performed under local or general anesthesia, depending on patient needs and surgical complexity. There are two primary types of transplants: full-thickness (penetrating keratoplasty) and partial-thickness (lamellar keratoplasty), each targeting different layers of the cornea. Surgeons use precise instruments, and in some cases lasers, to ensure accurate placement of the donor cornea. The graft is secured using fine sutures or other fixation methods. Patients usually experience only mild pressure during the procedure. Close monitoring during and immediately after surgery ensures the eye remains stable and reduces risks of complications.
Recovery and Postoperative Care
Healing after a corneal transplant requires patience and consistent care. Vision may remain blurry for several weeks or months as the eye adjusts to the new cornea. Eye drops are prescribed to prevent infection, reduce inflammation, and prevent graft rejection. Patients should attend all follow-up appointments to monitor progress and address any early signs of complications. Mild discomfort, light sensitivity, and redness are common during recovery. Protecting the eyes from injury and avoiding strenuous activity is essential during the healing period. Adhering strictly to postoperative instructions increases the chances of long-term graft success. Gradual vision improvement is expected, with many patients regaining significant clarity over time.
Tips for Maintaining a Healthy Graft
Proper care after surgery is critical to maintaining a healthy corneal transplant. Patients should follow these guidelines:
- Apply prescribed eye drops on schedule
- Avoid rubbing or touching the eyes
- Use protective eyewear during outdoor activities or while sleeping
- Attend all follow-up appointments
- Keep eyes clean and avoid exposure to dust or irritants
- Avoid heavy lifting or strenuous exercise for the initial months
- Maintain overall health and nutrition to support healing
Consistency in care supports the long-term survival of the graft. Patients who closely follow these guidelines are more likely to achieve optimal visual outcomes. Establishing a routine around eye care ensures the cornea remains protected. Awareness of proper care techniques reduces the risk of complications and enhances overall success. Over time, these habits become a natural part of maintaining eye health.
Vision Outcomes and Long-Term Prognosis
Many patients experience significant improvement in vision after a corneal transplant. The degree of improvement depends on the underlying condition and the type of transplant performed. Some patients may still require corrective lenses or additional procedures to achieve optimal clarity. Long-term graft survival relies on consistent medical care and protection of the eyes from trauma. Factors such as immune response, age, and overall eye health affect outcomes. Early detection of potential complications, such as graft rejection, can prevent permanent damage. With proper care, most corneal transplants provide lasting improvements in vision and quality of life.
Innovations in Corneal Transplantation
Modern advancements have transformed corneal transplant surgery. Minimally invasive techniques, such as endothelial keratoplasty and lamellar keratoplasty, target only the affected layers, reducing recovery time. Laser-assisted procedures increase precision and improve graft alignment. Artificial corneas and bioengineered grafts are emerging alternatives for patients without suitable donor tissue. Tissue preservation methods have also improved, ensuring high-quality donor corneas are available when needed. Ongoing research in immunology and rejection prevention continues to improve long-term success rates. These innovations make corneal transplants safer, faster, and more effective than ever before. Patients now have access to procedures that maximize both comfort and visual outcomes.
Common Misconceptions About Corneal Transplants
Several misconceptions about corneal transplants may cause unnecessary worry. Some patients believe the surgery is extremely painful, though most report only mild discomfort. Others assume graft rejection is inevitable, but adherence to medications significantly reduces this risk. Concerns about donor tissue availability are often overstated, thanks to modern eye banks. Many patients also expect instant vision improvement, not realizing that healing takes time. Believing that surgery carries high risk may prevent individuals from seeking treatment. By addressing these misconceptions, patients can approach corneal transplantation with confidence. Accurate knowledge encourages timely action and improves outcomes. Understanding the facts helps patients make informed decisions about their vision health.
Frequently Asked Questions About Corneal Transplants
How long does a corneal transplant last
With proper care, a transplant can last decades and continue providing clear vision
Is the surgery painful
Most patients experience minimal discomfort due to anesthesia and advanced surgical techniques
When can normal activities be resumed
Light activities may resume within a few weeks, while strenuous tasks may require several months of recovery
What are the signs of complications
Redness, pain, blurred vision, or sensitivity to light should be reported immediately
Will vision be perfect after surgery
Vision typically improves significantly, but some patients may still need glasses or contacts
Are there alternatives to corneal transplant
Specialized lenses or non-surgical therapies may help in mild cases, but severe damage usually requires surgery
How is donor tissue matched
Donor corneas are carefully screened and matched for compatibility to ensure safety and graft success
Takeaway
A corneal transplant is a transformative procedure for patients with severe corneal damage or vision loss. With careful evaluation, expert surgical care, and diligent postoperative management, most patients achieve significant improvements in sight and quality of life. Modern surgical techniques, enhanced tissue preservation, and ongoing research have made corneal transplantation safer and more effective than ever. Understanding the procedure, addressing myths, and adhering to medical guidance ensures optimal outcomes. For those struggling with vision impairment, exploring a corneal transplant with a qualified ophthalmologist offers hope for renewed clarity and independence.